Mobile Surgery Program

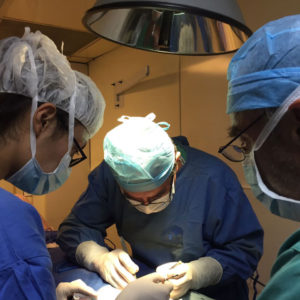
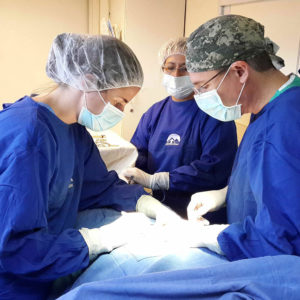
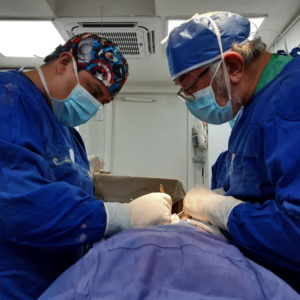
Cinterandes was founded in 1994, launching the first mobile surgery program of its kind in the world with an operating room built in the back of a truck. This program performs an average of 350 surgeries per year, in the most remote places of Ecuador and in the suburbs of cities.
With its mobile operating room, Cinterandes has visited 18 of the 24 Provinces of Ecuador, performing nearly 9,000 surgeries to date, traveling through the Andes mountains, the Pacific coast and the Amazon; on surgical missions with its volunteer medical staff, made up of Ecuadorian and foreign surgeons, anesthesiologists, residents and medical students, nurses and technicians, treating people who otherwise would not be able to access surgical services, in a safe way, close to the patient’s home, which means they don’t have to go far from home and travel long hours to be treated in big cities, humanizing medical service but with standards comparable to the best medical centers in the world.
Currently in our mobile surgical unit, we perform surgical interventions in the area of general surgery, such as: Laparoscopic cholecystectomy, tubal ligation, inguinal and abdominal herniorrhaphies, extraction of superficial tumors, circumcisions, orchidopexies, among others.
Medical missions in other provinces last four days and are coordinated in advance with a person from the community who is in charge of organizing on site. During the first day of the medical missions, all patients are screened, which together with the necessary medical exams, guarantees the safety of the process. Post-operative controls are carried out through Telemedicine. When the locations of the medical missions are remote and very poor, surgeries are free, thus maintaining the vision of our founder, Dr. Edgar Rodas Andrade: “The idea is that no one is denied access to surgery, because they do not have money”.
The Cinterandes mobile surgery program is internationally recognized and has been replicated in various parts of the world such as Africa. The program represents the best way of bringing surgical care to remote places or areas that do not have these health services, making surgery more humane and easily accessible for all, substantially improving the quality of life of hundreds of people annually.